Unfortunately, most of them didn’t achieve satisfactory results. Attenuation of inflammation can be achieved through inhibition of leukocytes activation, modification of macrophages polarization toward reparative phenotype, or deactivation of regulatory T cells. Over the last three decades, relentless efforts targeting at either reduction of the inflammatory pathways or activation of reparatory pathways have been performed in the aim of improving the prognosis of MI. Therefore, maintaining an appropriate and timely homeostasis balance between inflammatory and reparatory phases is crucial for the regeneration of the injured myocardium. Extensive experimental investigations demonstrated that prolonged and excessive inflammation resulted in accentuated injury and increased left ventricular adverse remodeling following MI. However, the duration and intensity of the inflammatory response determine the prognosis of MI. Inflammation is initiated to clear necrotic cell debris and extracellular matrix (inflammatory phase), then followed with fibroblasts transdifferentiation and scar formation (reparatory phase). Massive cell death occurs at the onset of infarction, which induces a drastic inflammation that is essential for cardiac repair, but is also involved in the pathogenic process of ventricular remodeling. We also outlined various approaches to enhance the curative effects of MSC-based therapy for MI patients. Here, we summarized current knowledge regarding the mechanisms of MSCs and their secretome mediated inflammation regulation for rejuvenating the infarcted myocardium. However, accumulating evidence indicated that MSCs conduct repair function through alternative modes including paracrine secretion of growth factors and inflammation-regulatory factors rather than engraftment and differentiation. Originally, direct differentiation to functional cells, such as endothelial cells, was considered to be the main mechanism for MSCs-mediated cardiac therapy. Undoubtedly, MSCs transplantation is a safe and promising approach for MI therapy. Mesenchymal stem cells (MSCs) have attracted much attention for their therapeutic potentials such as anti-apoptosis, immunomodulation, anti-inflammation, pro-angiogenesis and regeneration. In fact, cardiac inflammation is manipulated exquisitely by diverse crucial inflammatory cytokines and potentially reversible by regulating some of these factors, making it as a promising target for enhancing cardiac function. Accumulating reports have demonstrated the dual effects of inflammation on the cardiac repair, that is, clearing dead cells and debris in one way, and exacerbating damage if the inflammation is prolonged in the other way. Meanwhile, inflammation is initiated with the inflammatory cell infiltration, accompanied with the activation of both innate and adaptive immune responses. At the onset of MI, shortage of blood and oxygen supply undeniably induces the death of cardiomyocytes and other types of cells in the heart. Myocardial infarction (MI) remains a leading cause of death and emerges as a worldwide public health challenge in recent years. 
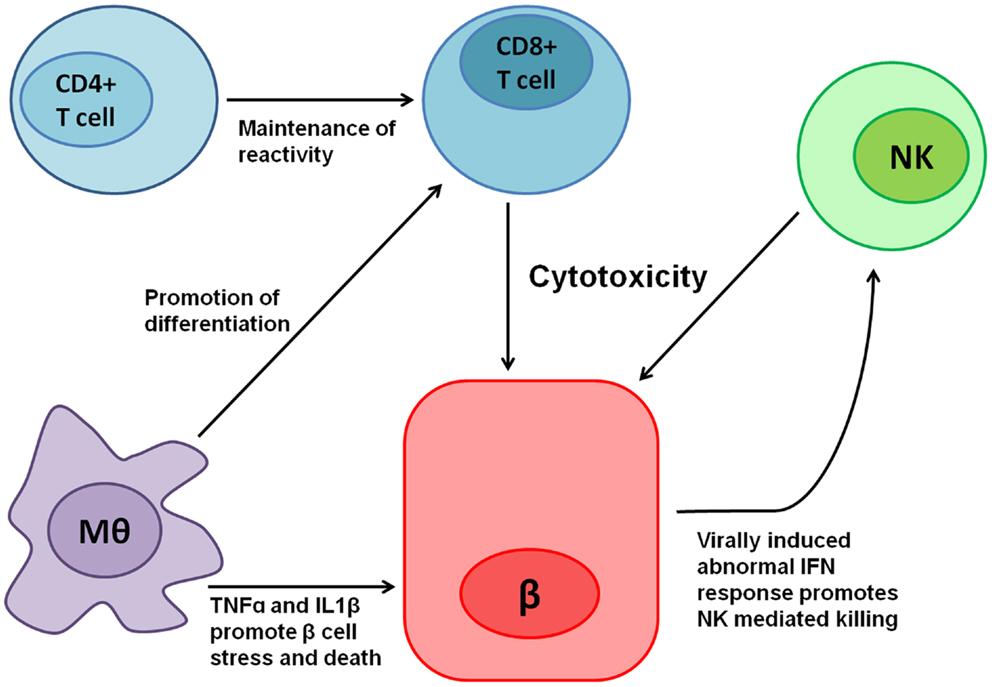
In this review, we provide an overview on the current understanding of the mechanisms on MSCs and their secretome regulating inflammation and immune cells after myocardial infarction and shed light on the applications of MSCs in the treatment of cardiac infarction. Many studies also proved that preconditioning of MSCs can enhance their inflammation-regulatory effects. In fact, transplanted MSCs have been shown to accumulate at injury sites of heart, exerting multiple effects including immunomodulation, regulating macrophages polarization, modulating the activation of T cells, NK cells and dendritic cells and alleviating pyroptosis of non-immune cells. Mesenchymal stem cells (MSCs) serve as an effective and innovative treatment option for cardiac repair owing to their paracrine effects and immunomodulatory functions. Inflammation plays crucial roles in the regulation of pathophysiological processes involved in injury, repair and remodeling of the infarcted heart hence, it has become a promising target to improve the prognosis of myocardial infarction (MI).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
